- Find a DoctorDoctors by Specialty
- Cardiac Electrophysiology
- Cardiology
- Colon & Rectal Surgery
- Family Medicine
- Gastroenterology
- General & Vascular Surgery
- Gynecological Oncology
- Gynecology
- Infectious Disease
- Internal Medicine
- Interventional Cardiology
- Interventional Radiology
- Nephrology
- Neurology
- Neurosurgery
- Obstetrics & Gynecology
- Oncology
- Oncology & Hematology
- Orthopedic Surgery
- Otolaryngology
- Perinatology
- Psychiatry
- Pulmonary Medicine
- Radiation Oncology
- Rheumatology
- Sleep Medicine
- Thoracic Surgery
- Urology
- View All Doctors
- Our ServicesMedical Services
- Bariatric Services
- Behavioral & Mental Health
- Breast Care
- Cancer Care
- Critical Care
- Ear, Nose, & Throat
- Emergency Services
- Gastroenterology
- Glossary
- Heart Care
- Home Care
- Hospice & Palliative Care
- Imaging & Diagnostics
- Long-Term Care
- Nephrology
- Orthopedics
- Primary Care
- Rehabilitation Therapies
- Robotic-Assisted Surgery
- Sleep Services
- Spine Care
- Stroke Care
- Surgery Services
- Telehealth Services
- Urology
- Urgent Care
- Virtual Urgent Care
- Women’s Services
- Wound Care
- Our Locations
- Patients & Visitors
- About Us
Content authored by Chelsea Johnson, MS, RD, LDN – Clinical Dietitian
 The Center for Disease Control (CDC) estimates 122 million Americans live with diabetes or prediabetes. The CDC also reported more than 1.7 million new cancer cases in one year in the United States. With these numbers, it is no surprise that patients come through the doors of the cancer center impacted by both cancer and diabetes.
The Center for Disease Control (CDC) estimates 122 million Americans live with diabetes or prediabetes. The CDC also reported more than 1.7 million new cancer cases in one year in the United States. With these numbers, it is no surprise that patients come through the doors of the cancer center impacted by both cancer and diabetes.
Many Patients Must Manage Both
Diabetes is a health condition that affects how food transforms into energy. When foods are digested, they are broken down into glucose (sugar) molecules. Glucose is your cells’ energy source. A healthy pancreas releases insulin to naturally move blood glucose (blood sugar) into cells. With diabetes, the pancreas either makes no insulin or your body cannot use insulin properly, creating a build-up of blood glucose in the bloodstream. There are different types of diabetes: pre-diabetes, gestational, type 1 diabetes, and type 2 diabetes. 90-95% of people have type 2 diabetes. Type 2 diabetes is heavily influenced by lifestyle factors like exercise, diet, stress, and weight.
In this blog, I’ll focus on type 2 diabetes. I hope to simplify the facts to help you feel more confident in managing diabetes with cancer.
The Connection Between Cancer and Diabetes
Controlling blood sugar helps improve wound healing, inflammation, quality of life, energy levels, and symptom management. All of these are important when tackling cancer treatment. Most importantly, managing blood sugar protects critical organs like the kidneys and heart.
Carbohydrate-heavy foods, steroids, and stress can cause high blood sugar. Not eating enough and exercising without enough fuel can cause low blood sugar. Think of it like a surfer riding waves- smoothly moving up and down over a continuous wave. That same motion, avoiding sharp drops and spikes, should mimic your daily blood sugar trends for best management. Cancer treatment throws curveballs at blood sugar control, which means it is important to monitor your numbers. It is not uncommon to need changes to oral medication or insulin during cancer treatment.
Here are some general guidelines on blood sugar checks from the American Diabetes Association (ADA):
- Before a meal, prick your finger or use a continuous glucose monitor (CGM). An appropriate number is between 80-130 mg/dL.
- 1-2 hours after a meal, prick your finger or use a CGM. An appropriate number should be less than 180 mg/dL.
- When your doctor checks your A1C, an average of your blood sugar over 3 months, the goal is less than 7%.
- If your blood sugar does not routinely fit into these ranges, notify your physician and dietitian.
Food Choices
I hear the same questions from patients: “What can I eat?” “What should I avoid?”. There is good news! All food groups provide quality nutrients and can be enjoyed with diabetes and cancer. Managing diabetes may mean you have to eat some foods less often or in smaller portions. Diabetes is not a “one-size-fits-all”. Set small, feasible goals that work best for you.
In general, two tools are used to help patients manage blood sugar through food choices:
1. The Plate Method
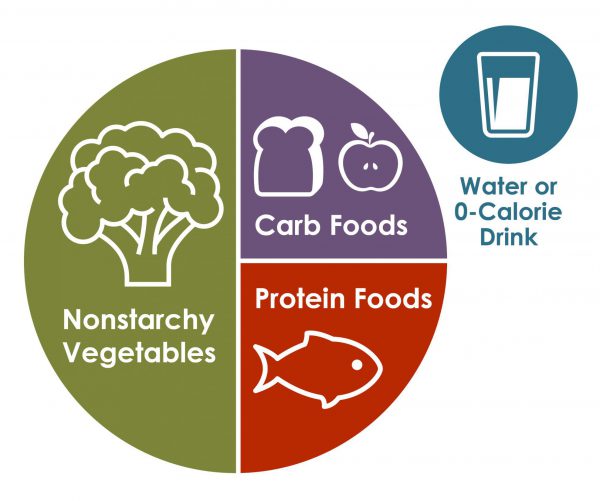
This method works best for visual learners. It is the simplest method. There are a few main concepts, helping simplify food choices using a plate. Fill half your plate with nonstarchy vegetables. Fill one-quarter of your plate with lean proteins. Fill one-quarter of your plate with carbohydrate foods. Choose water or a low-calorie drink.
This method highlights high protein and fiber-rich foods. These foods act as a buffer for rising blood sugar. These foods also help with muscle mass preservation and keeping stools regular during cancer treatment. Limit foods high in added sugars like cookies, cakes, and sodas. These foods raise blood sugar quickly. This does not mean you can never have them, just less often. Notice, these recommendations mimic the American Institute of Cancer Research (AICR) recommendations for cancer prevention. Tackle two health conditions with single lifestyle changes!
Click here to learn more about the Plate Method and food choices.
2. Carbohydrate Counting
 Tracking grams of carbohydrates helps control your blood sugar. For those of you who are planners, this method is great. If you take mealtime insulin, this is for you. Important note: carbohydrates are not the enemy. They are the mega fuel source for your whole body! The key to carbohydrate counting is planning to have about the same amount of carbohydrates at meals daily. Consistency is key. Nutrition Facts Labels actually list carbohydrates in each serving to help you count. This method encourages larger portions of lean proteins and low-carbohydrate foods while managing portion size and frequency of carbohydrate-rich foods. Since daily carbohydrate needs vary from one person to another, talk to your dietitian about creating an individualized plan.
Tracking grams of carbohydrates helps control your blood sugar. For those of you who are planners, this method is great. If you take mealtime insulin, this is for you. Important note: carbohydrates are not the enemy. They are the mega fuel source for your whole body! The key to carbohydrate counting is planning to have about the same amount of carbohydrates at meals daily. Consistency is key. Nutrition Facts Labels actually list carbohydrates in each serving to help you count. This method encourages larger portions of lean proteins and low-carbohydrate foods while managing portion size and frequency of carbohydrate-rich foods. Since daily carbohydrate needs vary from one person to another, talk to your dietitian about creating an individualized plan.
Learn more about carbohydrates and tracking here.
Practicing Self-Management
Self-management empowers patients to take control even when their health feels so out of control. Here are a few practical tips for self-management.
- Build a schedule for checking blood sugars. Keep a food and blood sugar log to share with your healthcare team.
- Try new recipes. Recipes can easily be modified to help with cancer treatment symptoms and controlling blood sugar. Check out powerhouse recipes for managing blood sugar.
- Use a Smartphone or other device to track food and activity goals. MyFitnessPal and MyPlate Calorie Counter are excellent free digital tools.
- Aim for a healthy body weight. Slight weight loss can have a huge benefit on blood sugar and cancer prevention. However, most providers want to see your weight remain stable during active cancer treatment. If you are interested in working on weight loss, ask your healthcare team for their recommendation.
- Get moving. Find activities you enjoy and tolerate on a schedule.
- Follow your doctor’s recommendation for pills and insulin shots. Sticking to your regimen lessens damage to organs affected by high blood sugar.
Additional Resources
Knox County Health Department (KCHD) offers a free 3-week diabetes education series on managing diabetes. You can work with a registered dietitian to learn about healthy eating and exercise, medications, and more. This class is open to everyone, regardless of their diabetes status. It is offered in English and Spanish. Click here for more information and registration. Reach out to your Thompson Cancer Survival Center registered dietitians to talk more about your health goals.
Visit the Thompson Cancer Survival Center Blog to explore other topics.
References
https://knoxcounty.org/health/diabetes_management.php
https://www.cdc.gov/diabetes/basics/diabetes.html
https://www.diabetesfoodhub.org/articles/what-is-the-diabetes-plate-method.html
https://www.cdc.gov/diabetes/managing/eat-well/diabetes-and-carbohydrates.html