Bariatric Surgery vs. Weight-Loss Drugs: What You Need to Know

- 9 minute read.
- Last Updated: 3/17/2026
GLP-1 injection pens are being used to treat both type 2 diabetes and obesity.
In recent years, type 2 diabetes injectables like Ozempic and other GLP-1 (Glucagon-like peptide 1) receptor agonists skyrocketed in use and popularity (due in large part to celebrity weight-loss endorsement and TikTok promotion), and transformed the treatment of obesity. Yet even with high-profile support of the ‘quick weight-loss fix’ that has taken the internet and social media by storm, there is still much to consider about the effectiveness of anti-obesity medications as a weight-loss solution, compared to alternatives like bariatric surgery.
What Are Weight-Loss Injectables and How Do They Work?
Approved in 2005 by the Food and Drug Administration, GLP-1 medications are known to treat type 2 diabetes by stimulating the body to produce more insulin, which in turn lowers blood sugar levels. In addition to stimulating the release of insulin, GLP-1 agonists also appear to curb hunger and delay gastric emptying, leading to potential weight loss.
Once prescribed by a doctor, these medications are typically self-injected once a week into the stomach, thigh or upper arm. Patients can dial the injection pen to provide the right dose and are cautioned against injecting medication into muscle or into the same place twice in a row.
Semaglutides vs. Tirzepatides: What’s the Difference?
Popular anti-obesity injectables like Ozempic, Zepbound, Wegovy and Mounjaro are all antidiabetic medications used for the treatment of type 2 diabetes and weight loss, but they feature different active ingredients. While brands like Ozempic and Wegovy contain semaglutide, other options like Zepbound and Mounjaro contain tirzepatide.
Ozempic (Semaglutide) mimics a hormone (glucagon-like peptide-1) that helps regulate glucose metabolism and appetite. By binding to GLP-1 receptors in the brain, Ozempic helps control appetite and reduce caloric intake.
Wegovy (Semaglutide 2.4 mg) is similar to Ozempic, but in a formula with a higher dose of GLP-1. The higher dose in Wegovy is believed to make it more effective.
Semaglutide Benefits
Clinical trials have shown that semaglutides can lead to substantial weight loss, often more than what patients have achieved with other weight-loss medications. It has demonstrated effectiveness in improving metabolic health and may be especially beneficial for individuals with obesity-related medical problems.
Mounjaro and Zepbound (Tirzepatides) increase insulin production and lower the amount of sugar produced by the liver. They work as appetite suppressants, slowing the food passing through the body, and making the patient feel fuller longer. Like Ozempic and Wegovy, tirzepatides target the glucagon-like peptide 1 (GLP-1) receptor agonists, but also target the dual glucose-dependent insulinotropic polypeptide (GIP). This makes tirzepatides the first weight-loss and diabetes medications “fighting on two fronts.”
Tirzepatide Benefits
With a double-punch treatment, tirzepatides have been shown to decrease how much you eat and increase the amount of energy you expend, which can result in weight loss.
Additional GLP-1 Receptor Agonists
Other GLP-1 receptor agonists are being explored for their potential in weight management. These medications use the body’s natural hormonal workings to regulate appetite and promote weight loss.
Exenatide: Available in both short-acting (Byetta) and extended-release (Bydureon) formulations, exenatide is another GLP-1 receptor agonist used in the treatment of type 2 diabetes. Studies have suggested its potential for weight loss, making it a medication of interest for those with obesity.
Liraglutide: In addition to its approval for managing diabetes, liraglutide (Saxenda) has been approved for chronic weight management in adults with a BMI of 30 or higher, or those with a BMI of 27 or higher with at least one weight-related medical condition. It is administered as a daily injection.
What is Bariatric Surgery and How Does It Work?
Bariatric surgery is recognized by the National Institutes of Health as the most effective long-term weight loss treatment for obesity. It includes several procedures, each designed to reduce the size of the stomach or alter the digestive process. There are four different bariatric surgery procedures:
Gastric Bypass Surgery (laparoscopic Roux-en-Y)
This procedure reduces the stomach through stapling and bypasses a portion of the small intestine, resulting in less calorie absorption.
Gastric Sleeve Surgery (laparoscopic sleeve gastrectomy)
This procedure removes approximately 85 percent of the stomach, which restricts the amount of food that can be eaten. Patients lose weight by eating fewer calories.
Biliary Pancreatic Diversion
This surgical procedure combines aspects of gastric bypass surgery and gastric sleeve surgery so that calories are incompletely absorbed, resulting in weight loss.
Laparoscopic adjustable gastric banding (LAGB)
In this procedure, an adjustable band is placed around the top of the stomach through small incisions in the upper abdomen, creating a small stomach pouch for a feeling of fullness after eating less food.
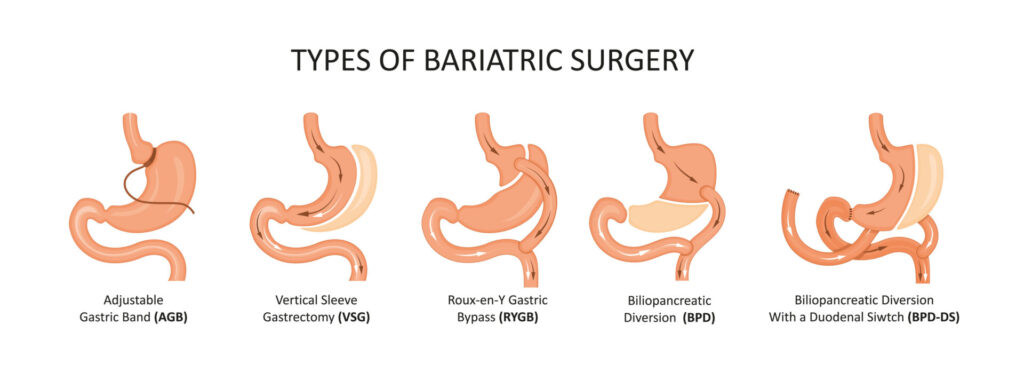
With the exception of the gastric banding procedure, the Covenant Health Bariatric Team performs most of these procedures laparoscopically using robotic-assisted technology, resulting in minimal scarring. Covenant Health bariatric surgeons no longer provide the gastric banding procedure because the band can erode or slip over time, and there is a higher risk of weight regain and re-operation.
How Do Weight Loss Drugs Compare to Bariatric Surgery?
Weight-loss medications and bariatric surgery have both proven effective in helping overweight and obese patients shed pounds and improve health. The idea of self-injecting medicine might not be a selling point for everyone, but the once-weekly or once-daily dosing of GLP-1s like Ozempic, Wegovy, Mounjaro and Zepbound makes them convenient and easy to manage. These medications also carry the possibility of side effects, and the weight loss may be short-term. Since they’re less likely to be covered by insurance, there is a long-term cost commitment. As a newer treatment for weight loss, these medications haven’t been as thoroughly researched as other weight-loss methods, although many studies are currently underway.
Bariatric surgery has been used for weight loss longer than the recently popularized GLP-1s, and board-certified surgeons have been safely performing the procedures for decades. These surgeons include bariatric experts at Covenant Health, where in most cases weight-loss surgery is covered by insurance when it has the potential to help patients medically. As with any surgery, bariatric procedures come with risks.
No matter what form of medically assisted weight loss you choose, be sure to have an open conversation with your healthcare provider to decide which option is best for you.
Who is Eligible for Weight-Loss Surgery Compared to Injectables?
Both weight-loss medications and bariatric surgery are typically reserved for patients who are classified as medically obese or for those with weight-related health conditions. A Body Mass Index assessment (BMI) can be a helpful tool in determining appropriate weight-loss strategies.
Eligibility for bariatric surgery often includes a Body Mass Index (BMI) over 35, combined with significant health issues like high blood pressure or diabetes, along with difficulty achieving and maintaining a healthy weight long-term.
The Food and Drug Administration (FDA) approves newer weight-loss medications for patients with a BMI of 30 or higher. The medications may also be prescribed for those with a slightly lower BMI who have medical conditions such as high blood pressure.
Insurerrs tend to follow similar guidelines, though some patients opt for “off-label” prescriptions by paying out-of-pocket when they don’t meet established criteria. Legislation to expand insurance coverage for GLP-1 medications is under consideration.
Effectiveness
No two cases are the same, so it’s important to understand that weight-loss results reported in case studies and clinical trials will vary depending on many factors. Talk to your healthcare provider or bariatric surgeon to set the most realistic short-term and long-term weight-loss expectations.
- Ozempic: In clinical studies, patients lost an average of 14 pounds in 30–56 weeks.
- Wegovy: Research reports weight loss of roughly 16 percent of a patient’s body weight or about 35 pounds after 68 weeks. Most of this weight loss occurs in the first 32 weeks.
- Mounjaro: Research indicates patients can expect to lose 20 percent of their total body weight in a little over a year.
- Zepbound: In a case study of more than 2,500 adults, participants saw an average weight loss of 15–22.5 percent.
- Gastric bypass surgery: It’s typical for patients to lose about 17 percent of their excess body weight during the first month after surgery and 65–70 percent in one or two years.
- Gastric sleeve surgery: Patients can usually expect to lose 55–60 percent of excess body weight in one or two years.
- Biliary Pancreatic Diversion: Patients are reported to have an average weight loss of 60–70 percent or more in five years.
- Laparoscopic Adjustable Gastric Banding: Patients are reported to have an average weight loss of 40–50 percent in two years.
Risks/Side Effects
Side effects of Ozempic and Wegovy may include nausea, diarrhea, gastroparesis and constipation, and can pose some risks to those who have a history of thyroid cancer or multiple endocrine neoplasia syndrome type 2.
Mounjaro and Zepbound can also have a range of side effects, some of them severe. Milder side effects typically include gastrointestinal problems like nausea, gastroparesis, constipation, diarrhea and abdominal pain. Among the more serious side effects are pancreatitis (swelling of the pancreas), hypoglycemia (low blood sugar) and severe allergic reaction. Very rare complications for GLP-1 agonists have included serious medical problems such as stomach paralysis and bowel obstructions.
Bariatric surgery, like any surgical procedure, carries inherent risks including infection, bleeding and adverse reactions to anesthesia. Given the altered anatomy and reduced food intake associated with bariatric surgery, individuals may risk malabsorption of micronutrients and minerals leading to nutritional deficiencies. Medically supervised nutrition with guidance from the bariatric surgeon and staff can help sidestep these deficiencies.
Cost
While in many cases bariatric surgery procedures are covered by insurance, most weight-loss medications are not. The American Society for Metabolic and Bariatric Surgery states the average cost of bariatric surgery ranges between $17,000 and $26,000. Because of the reduction or elimination of obesity-related conditions and associated treatment costs, it’s estimated that healthcare costs are reduced by 29 percent within five years of bariatric surgery.
In August of 2023, Becker’s Hospital Review reported that GLP-1 receptor agonists cost between $936 and $1,349 for a month’s supply. Becker’s Hospital Review also revealed that these drugs cost between five to 10 times more in the U.S. than other wealthy nations. Insurance may cover those who meet specific criteria, but many people opt to pay out-of-pocket for “off-label” prescriptions or generic alternatives so if they don’t meet the criteria.
Conclusion
Research and development to help patients overcome obesity and weight-related medical threats are constantly evolving and providing more promising options and outcomes. In addition, research has shown that semaglutide also can help prevent heart attacks and strokes. In 2024, the FDA approved Wegovy to help prevent life-threatening cardiovascular events in adults with cardiovascular disease who are obese or overweight. Early research has also shown that semaglutides may help lower the risk of Alzheimer’s in patients with type 2 diabetes. Research about the drugs’ potential for reducing inflammation in the brain and possibly preventing neurological conditions or diseases is ongoing.
When it comes to weight loss, however, neither medications nor bariatric surgery are “stand-alone” solutions. Each requires significant lifestyle changes for long-term success, including permanent changes in diet and regular exercise. Each works best with the support of healthcare professionals, family and friends long after the pounds come off.
If you’re having trouble losing weight, before you consider taking any new medications or make plans for bariatric surgery, talk to your healthcare provider about the potential risks and benefits.

About the Author
Covenant Health
Headquartered in Knoxville, Tennessee, Covenant Health is a not-for-profit, community-owned, healthcare enterprise committed to providing the right care at the right time and place. Covenant Health is the area’s largest employer and has more than 11,000 compassionate caregivers, expert clinicians, and dedicated employees and volunteers.

